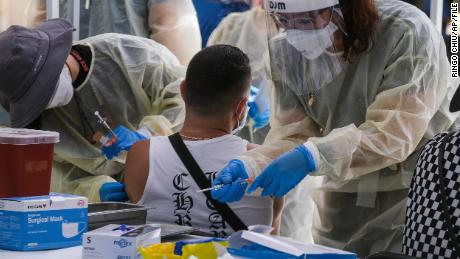
They put on face masks, and maintain a social distance from others, obeying the floor guidelines from the early days of the Covid-19 pandemic — when the determined want for vaccines far outweighed what federal and state governments may provide.
Many nonetheless will depart empty-handed as native hospitals and clinics have needed to rely on an inconsistent and inadequate provide of vaccines, a dilemma that has infuriated sufferers and advocates.
San Francisco General opens the clinic doorways at 8 a.m. and the line inches ahead slowly. The hospital will distribute the obtainable doses till the provide runs out.
For Cody Aarons, 31, it was his third try. He stood calmly with greater than 100 individuals already in entrance of him.
“I was in New York for the past month for work, and I tried with their online portal system and was unsuccessful in getting a vaccine,” mentioned the well being care employee who thought he might need a greater likelihood in San Francisco.
But 45 minutes after beginning the day’s distribution, a hospital employees member handed by with an announcement. “Folks we have reached our limit for today,” he shouted. “However, we will try to find you more shots.”
Although with no assure of getting the monkeypox vaccine that day, Aarons — and nearly everybody in line — stayed put.
“People want their vaccine,” mentioned Rafael Mandelman, a member of the San Francisco Board of Supervisors. “I know one person who was in that line four different days before he finally got his vaccination.”
Mandelman, who acquired up at 4:30 a.m. and waited for hours earlier than getting his vaccine shot days earlier, is pissed off with the rollout.
“After having come through a pandemic where we were able to discover a new vaccine, [and] distribute tens of millions of doses within a matter of months, the fact that with an existing known vaccine we cannot get more than these paltry little dribbles out is very frustrating to people,” he mentioned.
Desperate and fearful
For well being care employees, the outbreak is a irritating new chapter after the punishing Covid-19 pandemic.
“At the peak of Covid vaccinations, we averaged 1,400 to 1,500 (doses) a day. So we are completely used to the mass vaccination process,” nurse supervisor Merjo Roca mentioned.
But Roca and her employees are restricted in what they will do given the vaccine scarcity.
San Francisco well being officers initially requested 35,000 doses, however say they’ve solely gotten 12,000 from the federal stockpile. The state of California knowledgeable metropolis leaders that San Francisco will obtain 10,700 extra in the subsequent allotment, but there is not any clear indication when these doses will arrive or what number of will attain San Francisco General Hospital for distribution.
“I think one of our biggest challenges is really just the inconsistency of the supply,” Roca mentioned. “Our vaccine clinic prides itself on being able to help and vaccinate people when they come through our doors. So, it’s super hard for all of our staff not to be able to do that and have to turn people away and not even have information to say when we will get the doses next.”
With lots of these in line fearful about monkeypox’s fast rise in instances, the clinic employees really feel an added burden by not having the ability to ship for everybody.
“It’s very hard to listen to someone explaining why they want the vaccine and why they need the vaccine and we just don’t have it,” Roca added.
“It was like someone taking a hole-puncher all over my body”
The government argues it acted urgently and with the knowledge. And there are clear variations between the response now and the response to HIV/AIDS. But some advocates say the perceived lack of governmental urgency in addressing a public well being disaster that impacts queer communities at the moment mirrors what gay men have been experiencing a long time in the past.
Exchanges between then-President Ronald Reagan’s press secretary and reporters in 1982 and 1983 point out that the nation’s high officers and mainstream society considered the illness as a joke and never a difficulty of nice concern.
That stemmed from the notion of AIDS as a “gay plague” — a situation regarded as tied to the life and behaviors of gay men — regardless that instances had additionally been reported in ladies, infants, these with hemophilia and individuals who injected medication.
Now, greater than 40 years later, the gay neighborhood is as soon as once more grappling with feeling ostracized and neglected by their very own government.
“We have a responsibility to not further stigmatize or politicize this issue for a community that has long faced many issues, has long been marginalized in our community,” mentioned Tyler TerMeer, CEO of the San Francisco AIDS Foundation. “Dating all the way back to the earliest days of the HIV epidemic in our country, we saw our community abandoned by federal government in their response,” he mentioned.
The basis opened its doorways in 1982 “in a moment of crisis in our community, when the federal government abandoned us … there are parallels between that moment and this one,” in keeping with TerMeer.
“President Biden has called on us to explore every option on the table to combat the monkeypox outbreak and protect communities at risk,” mentioned White House National Monkeypox Response Coordinator Robert Fenton. “We are applying lessons learned from the battles we’ve fought — from COVID response to wildfires to measles, and will tackle this outbreak with the urgency this moment demands.”
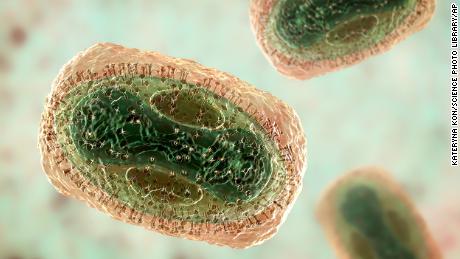
Monkeypox is a poxvirus, associated to smallpox and cowpox and it typically causes pimple- or blister-like lesions and flu-like signs akin to fever, in keeping with the CDC.
The lesions usually focus on the legs and arms, however in the newest outbreak, they’re exhibiting up extra continuously on the genital and perianal space, which has raised some considerations that monkeypox lesions could also be confused with STDs.
“I had between 600 to 800 lesions all over my body … It was like someone taking a hole-puncher all over my body. There were points where I couldn’t walk, couldn’t touch things,” mentioned Kevin Kwong, who just lately recovered from monkeypox after being recognized in early July.
He chronicled his ordeal on social media to convey consciousness to the outbreak and now needs to “focus on destigmatizing the gay community.”
According to the World Health Organization, there have been 25,054 instances confirmed by a laboratory as of August 3, and 122 possible instances.
But whereas the outbreak has disproportionately impacted some gay communities, there may be rising concern over the unfold of an infection.
“This is a reminder that everyone, regardless of age or sexual orientation, can get monkeypox if they come into contact with the virus,” the City of Long Beach cautioned, echoing CDC steerage that whereas the threat of an infection in kids is low, they’re “more likely to be exposed to monkeypox if they live in or have recently traveled to a community with higher rates of infection.”
“We need everyone to be rallying behind this issue and quickly,” TerMeer mentioned “There is an imminent window of time by which we can get ahead of the fast spread of monkeypox across our country and that window continues to close.”
CNN’s Harmeet Kaur, Augie Martin, Jen Christiansen, Carma Hassan, and Carolyn Sung contributed to this story.